Achilles Tendonitis Information
Overview
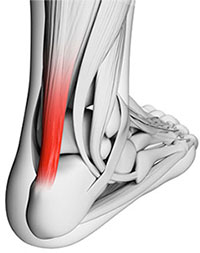
 Achilles Tendonitis is an inflammation of the Achilles Tendon. This tendon attaches the muscles in the calf of the leg to the back of our heels. The Achilles Tendon is a long and thick tendon, which moves our foot down, so that the toes point to the ground (plantar flexion). This tendon can become inflamed due to the following causes. Over utilizing it, such as too much running, especially up or down hill. Trauma, such as a kick to the tendon. Shoe or boot pressure, especially at its attachment to the heel, or just above it. There are over 250,000 injuries to the Achilles Tendon annually. In fact, more Than 10% of all running injuries are to the Achilles tendon. Tendonitis may be classified as either acute or chronic. Acute Achilles Tendonitis comes on quickly, usually after a specific activity or event. It is characterized by an overstretching or tearing of some of the small fibers of the tendon, and causes pain or tenderness when walking or running. It can occur at the insertion (near the attachment to the heel bone, or further up the leg, about 4 or 5 inches above the heel. Acute tendonitis can also follow a specific injury, such as a kick to the tendon while playing soccer. Chronic Achilles Tendonitis develops gradually over time. Many times, you can feel an obvious thickening of the tendon that may be tender when squeezed, due to long standing scarring of the tendon. Pain is also present when walking or during other forms of activity, and feels better at rest.
Achilles Tendonitis is an inflammation of the Achilles Tendon. This tendon attaches the muscles in the calf of the leg to the back of our heels. The Achilles Tendon is a long and thick tendon, which moves our foot down, so that the toes point to the ground (plantar flexion). This tendon can become inflamed due to the following causes. Over utilizing it, such as too much running, especially up or down hill. Trauma, such as a kick to the tendon. Shoe or boot pressure, especially at its attachment to the heel, or just above it. There are over 250,000 injuries to the Achilles Tendon annually. In fact, more Than 10% of all running injuries are to the Achilles tendon. Tendonitis may be classified as either acute or chronic. Acute Achilles Tendonitis comes on quickly, usually after a specific activity or event. It is characterized by an overstretching or tearing of some of the small fibers of the tendon, and causes pain or tenderness when walking or running. It can occur at the insertion (near the attachment to the heel bone, or further up the leg, about 4 or 5 inches above the heel. Acute tendonitis can also follow a specific injury, such as a kick to the tendon while playing soccer. Chronic Achilles Tendonitis develops gradually over time. Many times, you can feel an obvious thickening of the tendon that may be tender when squeezed, due to long standing scarring of the tendon. Pain is also present when walking or during other forms of activity, and feels better at rest.
Causes
As ?overuse? disorders, Achilles tendonitis and tendonosis are usually caused by a sudden increase of a repetitive activity involving the Achilles tendon. Such activity puts too much stress on the tendon too quickly, leading to micro-injury of the tendon fibers. Due to this ongoing stress on the tendon, the body is unable to repair the injured tissue. The structure of the tendon is then altered, resulting in continued pain. Achilles4Athletes are at high risk for developing disorders of the Achilles tendon. Achilles tendonitis and tendonosis are also common in individuals whose work puts stress on their ankles and feet, such as laborers, as well as in ?weekend warriors?-those who are less conditioned and participate in athletics only on weekends or infrequently. In addition, people with excessive pronation (flattening of the arch) have a tendency to develop Achilles tendonitis and tendonosis due to the greater demands placed on the tendon when walking. If these individuals wear shoes without adequate stability, their over-pronation could further aggravate the Achilles tendon.
Symptoms
Signs and symptoms of Achilles Tendinitis generally include pain and stiffness along your achilles tendon, especially in the morning. Pain in the back of your heel that gets worse with activity. Severe pain the day after exercising. Swelling that gets worse with activity. If you feel a pop in the back of your heel or bottom of you calf, you may have ruptured or torn you achilles tendon.
Diagnosis
The doctor will perform a physical exam. The doctor will look for tenderness along the tendon and pain in the area of the tendon when you stand on your toes. X-rays can help diagnose bone problems. An MRI scan may be done if your doctor is thinking about surgery or is worried about the tear in the Achilles tendon.
Nonsurgical Treatment
Physical therapy is the first and most useful defense for achilles tendonitis because of the two presentations outlined above. Treatments for the two types are quite different in approach. Midsubstance tendinitis responds well to stretching, whereas insertional tendnitis tends to be aggravated more by it. Depend on your trusted physical therapist to differentiate between the two and follow their guidelines on exercises and running modifications. Running gait patterns that show excessive ?sinking postures? tend to point to the source of achilles tendon problems. Altering your gait in the midstance phase of the cycle can reduce the load on the tendon dramatically and thereby reduce pain. Rely on your running physical therapist for proper guidance on altering your gait the right way. Stride Strong?s Portland Running Clinic gait analysis can identify and fix potential issues before pain sets in. Icing at the onset of acute achilles pain (i.e. when the injury is fresh and new) would help control the inflammation. Your next step should be to call our number for an appointment.
Surgical Treatment
Percutaneous Achilles Tendon Surgery. During this procedure the surgeon will make 3 to 4 incisions (approx. 2.5 cm long) on both sides of the Achilles tendon. Small forceps are used to free the tendon sheath (the soft tissue casing around your Achilles tendon) to make room for the surgeon to stitch/suture any tears. Skilled surgeons may perform a percutaneous achilles tendon surgery with ultrasound imaging techniques to allow for blink suturing with stab incisions made by a surgical suture needle. This procedure can be done in 3 different ways depending on the preference and experience of your surgeon. Instead of making several 2.5 cm incisions for this procedure, some surgeons will use guided imaging with an ultrasound to see the Achilles tendon tissue without having to open up your ankle. For this technique, they will use a surgical needle to repeatedly stab your Achilles tendon. These "stab incisions" will allow the surgeon to "blindly" suture your tendon without seeing the actual tissue. As another option - some surgeons will only make 1 to 3 incisions for smaller surgical implements to repair your tendon while relying on imaging ultrasound to see your damaged tissue. During either procedure the use of ultrasound imaging or endoscopic techniques requires a very skilled surgeon.
Prevention
Appropriately warm up and stretch before practice or competition. Allow time for adequate rest and recovery between practices and competition. Maintain appropriate conditioning, Ankle and leg flexibility, Muscle strength and endurance, Cardiovascular fitness. Use proper technique. To help prevent recurrence, taping, protective strapping, or an adhesive bandage may be recommended for several weeks after healing is complete.
 Achilles Tendonitis is an inflammation of the Achilles Tendon. This tendon attaches the muscles in the calf of the leg to the back of our heels. The Achilles Tendon is a long and thick tendon, which moves our foot down, so that the toes point to the ground (plantar flexion). This tendon can become inflamed due to the following causes. Over utilizing it, such as too much running, especially up or down hill. Trauma, such as a kick to the tendon. Shoe or boot pressure, especially at its attachment to the heel, or just above it. There are over 250,000 injuries to the Achilles Tendon annually. In fact, more Than 10% of all running injuries are to the Achilles tendon. Tendonitis may be classified as either acute or chronic. Acute Achilles Tendonitis comes on quickly, usually after a specific activity or event. It is characterized by an overstretching or tearing of some of the small fibers of the tendon, and causes pain or tenderness when walking or running. It can occur at the insertion (near the attachment to the heel bone, or further up the leg, about 4 or 5 inches above the heel. Acute tendonitis can also follow a specific injury, such as a kick to the tendon while playing soccer. Chronic Achilles Tendonitis develops gradually over time. Many times, you can feel an obvious thickening of the tendon that may be tender when squeezed, due to long standing scarring of the tendon. Pain is also present when walking or during other forms of activity, and feels better at rest.
Achilles Tendonitis is an inflammation of the Achilles Tendon. This tendon attaches the muscles in the calf of the leg to the back of our heels. The Achilles Tendon is a long and thick tendon, which moves our foot down, so that the toes point to the ground (plantar flexion). This tendon can become inflamed due to the following causes. Over utilizing it, such as too much running, especially up or down hill. Trauma, such as a kick to the tendon. Shoe or boot pressure, especially at its attachment to the heel, or just above it. There are over 250,000 injuries to the Achilles Tendon annually. In fact, more Than 10% of all running injuries are to the Achilles tendon. Tendonitis may be classified as either acute or chronic. Acute Achilles Tendonitis comes on quickly, usually after a specific activity or event. It is characterized by an overstretching or tearing of some of the small fibers of the tendon, and causes pain or tenderness when walking or running. It can occur at the insertion (near the attachment to the heel bone, or further up the leg, about 4 or 5 inches above the heel. Acute tendonitis can also follow a specific injury, such as a kick to the tendon while playing soccer. Chronic Achilles Tendonitis develops gradually over time. Many times, you can feel an obvious thickening of the tendon that may be tender when squeezed, due to long standing scarring of the tendon. Pain is also present when walking or during other forms of activity, and feels better at rest.
Causes
As ?overuse? disorders, Achilles tendonitis and tendonosis are usually caused by a sudden increase of a repetitive activity involving the Achilles tendon. Such activity puts too much stress on the tendon too quickly, leading to micro-injury of the tendon fibers. Due to this ongoing stress on the tendon, the body is unable to repair the injured tissue. The structure of the tendon is then altered, resulting in continued pain. Achilles4Athletes are at high risk for developing disorders of the Achilles tendon. Achilles tendonitis and tendonosis are also common in individuals whose work puts stress on their ankles and feet, such as laborers, as well as in ?weekend warriors?-those who are less conditioned and participate in athletics only on weekends or infrequently. In addition, people with excessive pronation (flattening of the arch) have a tendency to develop Achilles tendonitis and tendonosis due to the greater demands placed on the tendon when walking. If these individuals wear shoes without adequate stability, their over-pronation could further aggravate the Achilles tendon.
Symptoms
Signs and symptoms of Achilles Tendinitis generally include pain and stiffness along your achilles tendon, especially in the morning. Pain in the back of your heel that gets worse with activity. Severe pain the day after exercising. Swelling that gets worse with activity. If you feel a pop in the back of your heel or bottom of you calf, you may have ruptured or torn you achilles tendon.
Diagnosis
The doctor will perform a physical exam. The doctor will look for tenderness along the tendon and pain in the area of the tendon when you stand on your toes. X-rays can help diagnose bone problems. An MRI scan may be done if your doctor is thinking about surgery or is worried about the tear in the Achilles tendon.
Nonsurgical Treatment
Physical therapy is the first and most useful defense for achilles tendonitis because of the two presentations outlined above. Treatments for the two types are quite different in approach. Midsubstance tendinitis responds well to stretching, whereas insertional tendnitis tends to be aggravated more by it. Depend on your trusted physical therapist to differentiate between the two and follow their guidelines on exercises and running modifications. Running gait patterns that show excessive ?sinking postures? tend to point to the source of achilles tendon problems. Altering your gait in the midstance phase of the cycle can reduce the load on the tendon dramatically and thereby reduce pain. Rely on your running physical therapist for proper guidance on altering your gait the right way. Stride Strong?s Portland Running Clinic gait analysis can identify and fix potential issues before pain sets in. Icing at the onset of acute achilles pain (i.e. when the injury is fresh and new) would help control the inflammation. Your next step should be to call our number for an appointment.

Surgical Treatment
Percutaneous Achilles Tendon Surgery. During this procedure the surgeon will make 3 to 4 incisions (approx. 2.5 cm long) on both sides of the Achilles tendon. Small forceps are used to free the tendon sheath (the soft tissue casing around your Achilles tendon) to make room for the surgeon to stitch/suture any tears. Skilled surgeons may perform a percutaneous achilles tendon surgery with ultrasound imaging techniques to allow for blink suturing with stab incisions made by a surgical suture needle. This procedure can be done in 3 different ways depending on the preference and experience of your surgeon. Instead of making several 2.5 cm incisions for this procedure, some surgeons will use guided imaging with an ultrasound to see the Achilles tendon tissue without having to open up your ankle. For this technique, they will use a surgical needle to repeatedly stab your Achilles tendon. These "stab incisions" will allow the surgeon to "blindly" suture your tendon without seeing the actual tissue. As another option - some surgeons will only make 1 to 3 incisions for smaller surgical implements to repair your tendon while relying on imaging ultrasound to see your damaged tissue. During either procedure the use of ultrasound imaging or endoscopic techniques requires a very skilled surgeon.
Prevention
Appropriately warm up and stretch before practice or competition. Allow time for adequate rest and recovery between practices and competition. Maintain appropriate conditioning, Ankle and leg flexibility, Muscle strength and endurance, Cardiovascular fitness. Use proper technique. To help prevent recurrence, taping, protective strapping, or an adhesive bandage may be recommended for several weeks after healing is complete.